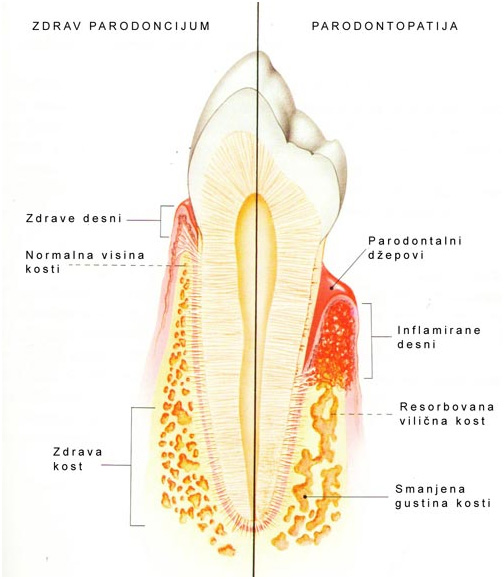
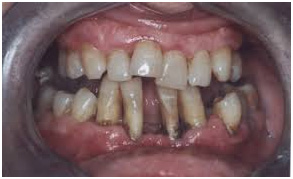
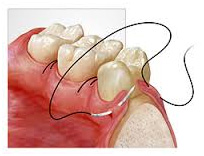
Parodontopathy is an inflammatory illness that attacks gingiva, alveolar bone and other structures of so called abutment tooth structure and is characterised with gingiva inflammation (gingivitis) and gingiva withdrawal, alveolar bone resorption, periodontal pockets and teeth dangling and falling out in terminal phase.
Parodnotopathy
The main etiological factor in formation of this disease are microorganisms in dental plaque. Some of them excrete extremely aggressive toxins and enzymes with which they damage the surrounding tissue and cause gingival inflammation. Gingival inflammation that is not cured attacks alveolar bone after a certain time which causes bone resorption and forming of periodontal pockets.
Although it can be agressive with tooth loss, parodonthopaty in the greatest number of cases is chronic and at the begining have almost unnoticable signs and symptoms.
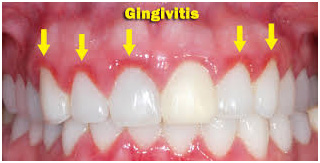
The first symptom patients usually notice is tooth brushing bleeding.Gingival bleeding is a sign of inflammatory process (gingivitis).
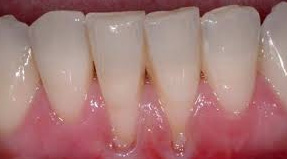
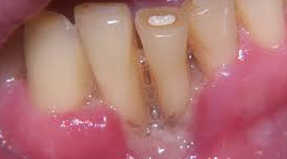
With the disease progression patients can notice that their gingiva has partially with rowen, that their tooth necks became bare, and that teeth react to termic and mechanical stimulus. In the advanced disease phase when there are a significant alveolar bone resorption and deep periodontal pockets patients notice that their teeth dangle, that there are gaps between them they hadn’t had before, or that the gaps they had have broaden, that some teeth have distorted, ”emerged” or come out of teeth line.
The therapy of parodontopathy
The therapy of parodontopathy is long-lasting and complex and requires patient’s active cooperation. Today we have a great range of therapy procedures that make it possible to control the disease, stop it or slow the great deal of its progression, even restore part of tissue lost during the disease which helps patients preserve natural dentition for years.
The treatment itself has several phases.
The first causal phase implies elimination of inflammation from parodontium.
Removing dental plaque, tooth scale, and other tooth films as well as all those local factors that precipitate their accumulation, and processing periodontal pockets eliminates the greatest number of microorganisms that caused inflammation and disease itself.
The second phase is surgical phase. With different types of so called slice procedure it is possible to significantly reduce depth of periodontal pockets and give gingiva changed morphology. Completeng bone defects with ”artificial bone” during scale surgery a part of lost bone is recovered and depth of periodontal pockets additionally reduced. Surgical therapy of parodontopathy also includes so called mucogingival surgery which is removal of mucogingival anomalies as well as aesthetic periodontal surgery that can repair some aesthetic defects that are result of the disease itself. Finally, surgical phase of therapy includes also preprosthetic parodontium preparing after which teeth are prosthetically recovered and occlusion and articulation stabilized. The last phase or the phase of conserving the reached results implies regular check-ups in order to perceive signs of possible new inflammation or disease recidive in time.